Hair Science, Scalp Health
PITYRIASIS AMIANTACEA
Pityriasis amiantacea is a condition in which there is excessive scaling of the scalp. Thick silvery or yellowish scales encircle the hair shafts and may bind down tufts of hair. The scales may resemble asbestos, giving rise to the term amiantacea – the French word for asbestos is ‘amiante’.
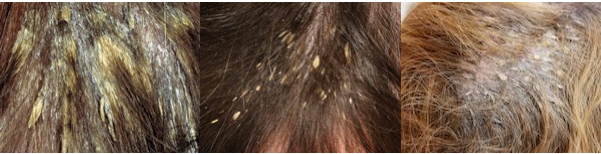 Pityriasis amiantacea
Pityriasis amiantacea
What is the cause of pityriasis amiantacea?
Pityriasis amiantacea is a reaction pattern rather than a specific diagnosis. Common conditions that may present with pityriasis amiantacea include:
- Scalp psoriasis
- Seborrhoeic dermatitis
- Atopic dermatitis
- Tinea capitis.
Head lice and lichen simplex should also be considered. When no underlying cause is found, the condition is often called idiopathic pityriasis amiantacea.
Clinical features
Pityriasis amiantacea more often affects females than males. It is generally seen in children and young adults. It is characterised by thick scales wrapping around and binding down tufts of hair. The scaling may be localised or generalised depending on the underlying condition and its duration. It may be complicated by secondary staphylococccal infection (impetiginisation), when the skin becomes sticky, oozy and crusted. Temporary or permanent hair loss (alopecia) may also occur. If the underlying skin condition is not clear, the entire skin should be examined to uncover the cause of pityriasis amiantacea. This enables targeted therapy against the specific disease and prevents long term complications such as permanently bald areas.
Identifying the cause of pityriasis amiantacea
Skin condition
Description
- Well-defined red scaly plaques on elbows and knees (chronic plaque psoriasis)
- Red shiny patches in skin folds (flexural psoriasis)
- Nail pitting, yellowing or thickening due to nail psoriasis
- Psoriatic arthritis Seborrhoeic dermatitis
- Patches similar to psoriasis but less well-defined and less red
- Scale tends to be yellowish in colour
- Affects eyebrows, nasal crease, behind the ears and chest Atopic dermatitis
- Usually starts in infancy
- Skin folds of arms and legs often affected
- May have generally itchy dry skin
- Flare-ups result in red, blistered, scratched patches Tinea capitis
- Fungal culture reveals dermatophyte fungus
- Localised scaly bald patches
- Broken off or loose hairs
- There may be cervical lymph node enlargement Head lice
- Egg cases on hair shaft (nits) and scurrying lice
- Prominent on back of neck and behind ears
- There may be cervical lymph node enlargement Lichen simplex
- Localised itchy dry patch of skin
- Often at back or one side of scalp
- Thickened, darkened plaques with broken-off hairs due to scratching
What investigations should be done?
Skin and hair samples for mycology and bacterial culture may be useful. Skin biopsy is rarely necessary.
Treatment Treatment depends on the specific underlying disease.
- Mineral or vegetable oils especially olive oil may help to loosen the adherent scales.
- Washable leave-on creams or wash-off shampoos containing salicylic acid, coal tar and sulphur may be of help in reducing the scaling and inflammation, e.g. coconut compound ointment.
- Intermittent courses of topical steroids are useful for psoriasis and various types of dermatitis, often as lotions or gels.
- Antifungal shampoo (e.g. ketoconazole or ciclopirox) is often prescribed and may be helpful for underlying seborrhoeic dermatitis.
- Oral antifungal agents are necessary for confirmed tinea capitis infection.
- Oral antibiotics may be prescribed for bacterial infection. Idiopathic pityriasis amiantacea often clears completely with treatment and does not recur. Tinea capitis may be cured by appropriate antifungal treatments. However, pityriasis amiantacea or less severe scalp scaling tends to persist or reappear when it is due to a chronic skin condition such as psoriasis or seborrhoeic dermatitis.
Scalp Health Active Botanicals


THYME
Thyme Oil has an anti-bacterial effect due to its high content of phenol (antiseptic) and is used for this benefit in scalp care preparations.


CHAMOMILE
(Bisabolol) A clinically tested active; Bisabolol protects and heals the skin from the effects of daily stress. It is a naturally occurring active ingredient found in chamomile that accelerates the healing process.


ALLANTOIN
(Comfrey) A clinically tested soothing, softening and protective active as found in the comfrey plant. It improves the skin's moisture retention providing a smoothing effect. It exfoliates dry and damaged cells increasing softness and a radiant appearance. It helps with the prevention of scalp irritation and supports the natural regeneration of the skin/ scalp.










