Hair Science, Hair Concerns, Hair Loss Women
OVERVIEW OF HAIR LOSS
 GENERAL OVERVIEW OF TYPES OF HAIR LOSS AND ALOPECIA TELOGEN EFFLUVIUM
GENERAL OVERVIEW OF TYPES OF HAIR LOSS AND ALOPECIA TELOGEN EFFLUVIUM
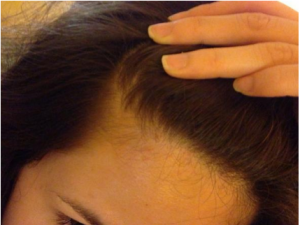
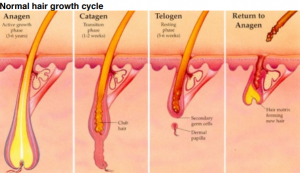
Telogen effluvium is a form of diffuse hair loss that occurs during the ‘telogen’ or ‘resting’ phase of the hair growth cycle. Telogen effluvium can be either acute or chronic depending on the cause and severity of the disturbance. Diffuse hair loss usually takes place around 8-12 weeks after the event which triggered it, so you may not always connect the two. If you notice excessive hair shedding, look back a couple of months for possible causes or events in your life which may explain the change. On average, it is OK to lose up to 100 hairs a day provided they are growing back. However, telogen effluvium can result in as many as 300 hairs being shed in a 24 hour period.
WHAT CAUSES TELOGEN EFFLUVIUM?
Telogen effluvium can be caused by a wide range of factors including iron deficiency, ferritin (stored iron) deficiency, protein deficiency, shock, rapid weight loss, stress, flu, pregnancy and menstrual problems.
 TREATMENT FOR TELOGEN EFFLUVIUM
TREATMENT FOR TELOGEN EFFLUVIUM
Telogen effluvium resulting from short-term illness, or a sudden medical issue which is not permanent, will usually resolve itself. However, chronic telogen effluvium due to nutritional deficiencies often needs to be treated with the appropriate nutritional supplements. Blood tests can be very helpful in diagnosis and should always be carried out if you have noticed increased hair loss for longer than 4 weeks. Hair lost during telogen effluvium almost always grows back once the underlying issue has been resolved.
FOLLICLE SENSITIVITY
Follicle sensitivity means follicles that are sensitive to the action of androgens (male hormones).
This sensitivity is not simply ‘caught’ or randomly acquired, but genetically inherited and has been there since birth. It is important to realise that if you have follicle sensitivity, normal or even sub-normal amounts of circulating androgens can cause hair loss. However, if you have little or no hair follicle sensitivity, then your hair may not be unduly affected by extra circulating androgens. This plays an important role in many types of hair loss from hair loss caused by PCOS, contraceptive pills and stress, to gradual genetic thinning and male pattern hair loss. As well as having the ability to affect hair on your scalp, androgens can also influence the growth of hair on the rest of your body, resulting in extra hair in male areas such as the face on females. If you have follicle sensitivity you may notice excess body and facial hair, and this is true of both men and women.
 TREATING FOLLICLE SENSITIVITY
TREATING FOLLICLE SENSITIVITY
There is no cure for follicle sensitivity, but topical and oral treatments are available that can help reduce the action of androgens on hair follicles. Or for women, treatments that decrease the amount of circulating androgens if levels are above the normal range. Often the two methods used in conjunction are most effective.
ANDROGENIC ALOPECIA
Hair thinning, ie a gradual reduction in the diameter of individual hairs, can be caused by a number of factors, the most common being ‘androgenic thinning’. With androgenic thinning, the growth (anagen) phase of your hair cycle becomes shorter and shorter, and the hair also grows back progressively finer. Hair thinning can occur on its own or alongside increased hair shedding. Androgenic thinning is related, as the name implies, to androgens (male hormones) and is genetically determined. What may (or may not!) surprise you is that both men and women have androgens. However, the levels are higher in men. It is when there are above average levels in women that
hair follicles become affected. Androgenic hair thinning is usually more common, and noticeable, in men than in women due to the higher levels of male hormones. The pattern of loss can also be different. However, genetic hair thinning is not only related to how high your male hormone levels are, but also to how sensitive your follicles are to them.
 ALOPECIA AREATA
ALOPECIA AREATA
‘Alopecia’ is a general term for hair loss – from mild and temporary shedding to profuse and permanent loss. It is the preceding word which explains the type of hair loss – in this case ‘areata’, which means ‘in
areas’. Alopecia areata causes specific areas of baldness that appear randomly throughout your scalp. This hair loss can be temporary, semi-permanent (recurring) or permanent, and can also affect facial (beard) hair in men, and eyebrows, eyelashes and body hair in both sexes. It can cause total loss of hair on the head, ‘alopecia totalis’, or very rarely leads to a universal loss of hair, or ‘alopecia universalis’.
HOW COMMON IS ALOPECIA AREATA?
Alopecia areata affects approximately 4% of the population (90,000 in the UK alone), and around 98% of those diagnosed recover. Alopecia areata can affect all ethnic groups and ages, but is most likely to occur between the ages of 20 and 50. It also occurs equally in both men and women.
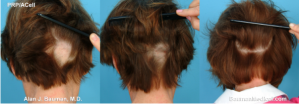
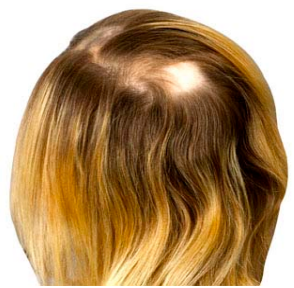
WHAT DOES ALOPECIA AREATA LOOK LIKE?
The main feature of alopecia areata is the presence of bald patches surrounded by little ‘exclamation mark hairs’. They are thicker at the top and taper to a thinner end, with the root a blob at the bottom. The number of exclamation mark hairs you have can indicate how active the alopecia areata is – in general the more there are, the more rapid its progress. However, sometimes there are no visible exclamation mark hairs at all – in these cases, alopecia areata may be diffuse (spread over a large area), but this is rare. In alopecia there is also inflammation present at the lower end of the hair follicle, but you can’t see it. Rarely, small patches of alopecia areata can grow, overlap and progress to total baldness, or alopecia totalis.
CAUSES OF ALOPECIA AREATA
Alopecia areata is widely accepted to be an autoimmune disorder, where your body sees certain hair cells as foreign enemies and attacks them. What triggers this response isn’t entirely understood, but 90% of cases are associated with stress, shock, bereavement or an accident and/or illness. There is also often a genetic predisposition and there are in fact several reported cases of alopecia areata’s occurrence in twins. Alopecia areata is also more common in those that suffer from hayfever, eczema, Addison’s Disease, pernicious anaemia, rheumatoid arthritis, ulcerative colitis, lichen planus, diabetes mellitus, vitiligo, lupus and thyroid disease.
TREATMENT
In many cases, alopecia areata spontaneously resolves itself within a year, but there are also treatments available to help bring about remission.
CORTICOSTEROID INJECTIONS
Corticosteroid injections are thought to be the most effective of treatments for alopecia areata, especially when used on small patches. They are given every few weeks, and can be used to treat bald areas on your scalp, eyebrows and body.
HOW THEY WORK
They suppress your body’s immune system, so that it no longer attacks your hair follicles. SIDE EFFECTS Pain at the injection site and thinning of the skin.
TOPICAL CORTICOSTEROIDS
The benefits of topical corticosteroids are debatable. They are applied daily to affected scalp areas, but cannot be used on the face or body. Possible topical creams and gels include: betamethasone, hydrocortisone and mometasone.
HOW THEY WORK
Similar to corticosteroid injections, but applied differently.
SIDE EFFECTS
Acne and thinning of the skin.
 ULTRA-VIOLET RAYS
ULTRA-VIOLET RAYS
Can Inflame your scalp, like a sunburn. How they work: They focus your immune system on the hair cells affected by the UV, which can allow the air to regrow. Simply put, cells go to repair the damaged skin and ‘trick’ your hair into growing. It is important to recognise that there is currently no cure for alopecia areata, and it often resolves by itself. However in some cases, even with treatment, it still recurs. Some people seem to be more prone to alopecia areata, and maintenance treatment is recommended and helpful. We often rule out transplants for treatment of alopecia areata. Transplants aren’t a solution as one never knows where alopecia areata will strike and it can recur and affect transplanted hairs as well as nontransplanted hairs. While you can still have transplants done, if the alopecia then affects those areas it can cause even more psychological and emotional distress.” It is also possible to apply small amounts of ‘Deep Heat’, rubbed into the affected areas; this will increase blood flow and circulation to the area, giving/increasing the possibility of stimulated hair growth.
 TRACTION ALOPECIA
TRACTION ALOPECIA
Traction alopecia is hair loss caused by a constant pulling on the hair (and hence the hair follicles). It is most commonly seen in women who wear weaves and hair extensions, but also occurs in those who consistently wear their hair pulled back tightly from their scalp, like ballerinas and gymnasts, and also from excessive or harsh brushing and/or backcombing. At first traction alopecia from hair extensions, weaves and incorrect styling is reversible; you can stop the process or take them out and your hair will grow back. However, over time irreversible damage can be done if the hair starts to grow back and is pulled out again and again. This happens because the constant pulling of the hair from its follicle eventually weakens the growth of the hair, which can cause your hair to grow back finer or even to not grow back at all.
TRAUMATIC/SCARRING ALOPECIA
Permanent, scarring alopecia is a ‘secondary’ cicatricial alopecia and is caused by external damage to hair follicles. These include damage from cosmetic burns from hot combs, straightening irons, radiotherapy, chemical straightening and also from trauma involving the scalp (such as car accidents or a bad fall). Although rare, permanent hair loss from these methods can either be an immediate bald patch, or cumulative hair loss from repeated damage.
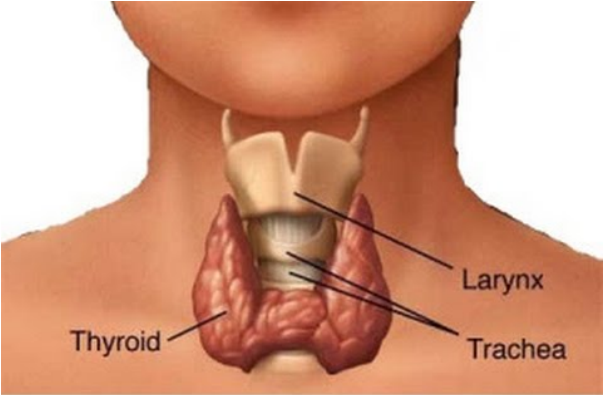 THYROID DYSFUNCTION
THYROID DYSFUNCTION
The thyroid is a gland that regulates your metabolism. Your thyroid can be affected by many conditions. These include, but are not limited to, nutritional deficiencies, pregnancy and menopause. Thyroid problems can also be caused by medications you are taking, or may simply be genetic and/or part of an underlying condition.
WHY THYROID FUNCTION IS IMPORTANT TO YOUR HAIR
Thyroid function is important to your hair as it helps to control the production of proteins and also your body’s use of oxygen. Having either a hypothyroid (low) or a hyperthyroid (high) can cause hair loss, hair thinning or reduced hair growth, and, when severe, hypothyroid causes hair loss in up to 50% of cases. Both hypo and hyperthyroid are easily diagnosed by low or high thyroid test readings. However, readings just within the normal range (such as high-normals and low-normals) should also be looked at if you are experiencing hair loss.
THYROID CONDITIONS
Two common thyroid diseases are Hashimoto’s (hypo) and Grave’s (hyper). Hair loss is just one of the symptoms of these and you would expect to experience one or more of the others listed below.
SYMPTOMS OF HYPERTHYROID
High blood pressure Rapid heartbeat Increased sweating Insomnia Weight loss (despite increased appetite) Bulging eyes Hair thinning
SYMPTOMS OF HYPOTHYROID
Slower pulse Hoarse voice Intolerance to cold Weight gain Some loss of eyebrow hair Thinner and dryer hair If you begin to notice any of these symptoms, we suggest you consult with your doctor.
TREATMENT I
suggest you make an appointment to see your doctor and/or endocrinologist if you suspect you have hyper- or hypothyroid. There are many medications that treat thyroid disorders, but they are prescription only. Once your thyroid is being treated by your doctor, there are specialized, hand-made hair products we can prescribe to help promote regrowth and combat hair loss. We will also be able to consult with your other specialists in order to establish the best treatment route for both your body and your hair.
Volume-ise / Hairfood Active Botanicals


GINGKO
Working with Kigalia and Clary as an original blend of 3 plants acting synergistically and allowing scalp toning and limiting hair loss. They act on factors avoiding hair loss including 5-alpha-reductase inhibition, scalp microcirculation improvement and to decrease inflammation contributing to Seborrhoea (oiliness) which can block scalp follicles inhibiting growth.


KIGALIA AFRICANA
Working with Gingko and Clary as an original blend of 3 plants acting synergistically and allowing scalp toning and limiting hair loss . They act on factors avoiding hair loss including 5-alpha-reductase inhibition, scalp microcirculation improvement and to decrease inflammation contributing to Seborrhoea (oiliness) which can block scalp follicles inhibiting growth.


CLARY
Working with Kigalia and Gingko as an original blend of 3 plants acting synergistically and allowing scalp toning and limiting hair-loss. They act on factors avoiding hair loss including 5-alpha-reductase inhibition, scalp microcirculation improvement and to decrease inflammation contributing to Seborrhoea (oiliness) which can block scalp follicles inhibiting growth.











