Hair Science, Colour Processing, Hair Concerns
PPD DYES
What is paraphenylenediamine and where is it found?
Paraphenylenediamine (PPD) is a chemical substance that is widely used as a permanent hair dye. It may also been found in textile or fur dyes, dark coloured cosmetics, temporary tattoosphotographic developer and lithography plates, photocopying and printing inks, black rubber, oils, greases and gasoline. The use of PPD as a hair dye is popular because it is a permanent dye that gives a natural look. Hair can also be shampooed without becoming decoloured and perming to achieve waves or curls can be done without difficulty. PPD hair dyes usually come packaged as 2 bottles, one containing the PPD dye preparation and the other containing the developer or oxidizer. PPD is a colourless substance that requires oxygen for it to become coloured. It is this intermediate, partially oxidised state that may cause allergy in sensitive individuals. Fully oxidized PPD is not a sensitiser thus individuals with PPD allergy can wear wigs or fur coats dyed with PPD safely.
 What are the reactions to PPD allergy?
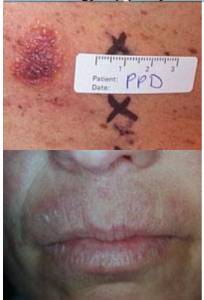
What are the reactions to PPD allergy?
Reaction caused by the use of hair dye in mild cases usually only involves dermatitis to the upper eyelids or the rims of the ears. In more severe cases, there may be marked reddening and swelling of the scalp and the face. The eyelids may completely close and the allergic contact dermatitis reaction may become widespread. Severe allergy to PPD can result in contact urticaria and rarely, anaphylaxis. People working with PPD such as hairdressers and film developers may develop dermatitis on their hands; patch testing usually reveals hypersensitivity to PPD. Occupational allergy to PPD has been found in a milk tester whom through laboratory work was in frequent contact with PPD solution. Dermatitis on the hands and occasional spreading to the arms and upper chest occurred. PPD has also been suspected of precipitating contact leukoderma and vitiligo in genetically predisposed individuals.
Contact allergy to p-phenylenediamine
Am I allergic to PPD?
Most hair colour preparations, particularly those containing PPD, carry a warning on the packaging to the effect that a patch test should be done prior to use of the dye. There are basically 2 patch testing methods available to test for allergic sensitivity to PPD.
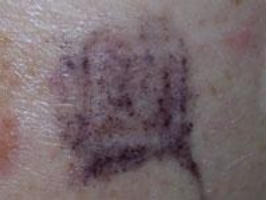 Patch test method 1: uncovered Patch test method 2: covered
Patch test method 1: uncovered Patch test method 2: covered
- Routine technique used by consumers for testing hair dye sensitivity
- Instructions for testing should be included with every package of hair dye preparation
- Essentially the test involves applying a 20 cent sized spot of solution (i.e. dye and developer mixed together) to either the neck (behind the ear) or the inner bend of the elbow. Allow to dry and leave uncovered for 48-72 hours. If no irritation or rash occurs during this time then the test is negative and one can assume that the risk of developing a rash will be much less when the dye is applied to the whole head.
- Any immediate signs of irritation or rash are more likely to be an irritant contact dermatitis (i.e. nonallergic)
- A 1+ to 2+ reaction (scale measuring PPD sensitivity) to PPD hair dye usually indicates that dermatitis will develop if the mixture is used
- Diagnostic test used to determine PPD sensitivity
- Patch testing using 2% PPD in petrolatum
- A +/- reaction (scale measuring PPD sensitivity) to this patch test method usually means that these individuals can use PPD hair dyes without difficulty
- A 1+ to 3+ reaction indicates allergic dermatitis will most likely occur with use of hair dyes thus preventing their use • Positive reaction from both methods provides confirmation that PPD is the cause of dermatitis and PPD containing products should be avoided
Treatment of PPD dermatitis
In acute severe cases of PPD hair dye dermatitis, wash the hair and scalp thoroughly with a mild soap or soapless shampoo to remove the excess dye. Apply a 2% hydrogen peroxide solution or compresses of potassium permanganate in a 1:5000 dilution to completely oxidise the PPD. To soothe, soften the crust and alleviate the tight feeling of the scalp, a wet dressing of cold olive oil and lime may be used. Further treatment with a topical application of an emulsion of water and water-miscible corticosteroid cream, or oral corticosteroids may be indicated. Management of PPD dermatitis on other parts of the body may be treated as for any acute dermatitis/eczema; this may include treatment with topical corticosteroids and emollients.
What should I do to avoid PPD allergy?
If you have an allergy to PPD and have your hair dyed, you should avoid the use of all oxidation type hair dyes. These are usually recognised by coming in a 2-bottle preparation. Inform your hairdresser that you are allergic to PPD. Semi-permanent hair dyes may be a suitable alternative but approximately 10% of individuals who are allergic to PPD also react to these; patch testing to confirm sensitivity should be performed prior to their use. Metallic hair dyes and vegetable rinse hair dyes may be used but these do not provide permanent colouring. Some newer permanent and semipermanent hair dyes use para-toluenediamine sulfate (PTDS) instead of PPD. This is likely to be tolerated by about 50% of people who are allergic to PPD. Patch testing is recommended prior to use. In cases of occupational exposure, avoid contact with PPD by wearing suitable protective garments such as gloves and protective sleeves. Alert your doctor or dentist to the fact that you have an allergy to PPD, this is particularly important if you a receiving treatment which may require the use of a local anaesthetic. Allergy to PPD may make you sensitive to other related compounds. As a precaution you should avoid using products containing any of these substances.
Related substances to PPD which may also cause an allergic reaction
- Azo dyes: used in semi-permanent and temporary hair dyes, ballpoint pen inks, gasoline and diesel oil, and as colouring agent in foods and medications
- Benzocaine and procaine: these are local anaesthetics used by doctors and dentists
- Sulfonamides, sulfones, sulfa drugs: PPD allergy may make you sensitive to the use of these drugs also, discuss with your doctor before changing or stopping your medication
- Para-aminobenzoic acid (PABA): this is used in sunscreens and creams that are readily available in over-the-counter preparations. You should only used sunscreens that are labeled ‘PABA-free’. Ask your pharmacist for suitable alternatives.
- Para-aminosalicylic acid: used for tuberculosis
Your dermatologist may have further specific advice, particularly if you are highly sensitive to PPD.
Alternative names for paraphenylenediamine
- PPD or PPDA
- Phenylenediamine base
- p-Phenylenediamine
- 4-Phenylenediamine
- 1,4-Phenylenediamine
- 4-Benzenediamine
- 1,4-Benzenediamine
- para-Diaminobenzene (p-Diaminobenzene)
- para-Aminoaniline (p-Aminoaniline)
- Orsin™
- Rodol™
- Ursol™
Further information
Formula:4-Phenylenediamine base – C6H8N2
CAS number: 106-50-3 Cross reactions:
- Azo and aniline dyes
- Benzocaine
- Procaine
- Para-aminobenzoic acid (PABA)
- Para-aminosalicylic acid
- Sulfonamides
- Carbutamide
- Hydrochlorothiazide
Appearance: White to slightly red solid crystals that darken on exposure to air.
Sensitizer: intermediate, partially oxidised PPD
Patch Test: 2% PPD in petrolatum
Reference
Book: Fisher’s Contact Dermatitis. Ed Rietschel RL, Fowler JF. Lippincott Williams & Wilkins 2001 PPD DYES There has been a lot of talk over the years of PPD or paraphenylenediamine, Ppd is a chemical agent that is present in many permanent hair colours. PPd’s are popular as they give colour good coverage, integrity and facilitate a natural looking shade of colour. The downside is that they are potentially sensitising, and therefore can cause allergic reaction in rare cases to an individual. The reaction can range from minor irritation and tingling to an anaphylactic shock. Whilst allergic reactions are rare (about 250,000 to 1) they can occur and you need to be aware. Now more than ever a patch test before you have a new colour or colour in a new salon or dare I say it colour you have purchased to do at home. Simply, take a small amount of the colour (the salon will do this for you) and apply to two places, either the back of your ear, the underside of your wrist, or the crease in your elbow. During the next 24 hours wait to see if there is any reaction. If there is not it is usually fair to assume that you may continue with your colouring. I would like to point out that I recommend that this should be done evert time you colour your hair even in the same salon using the same colour or at home using the same colour. The body is a finely balanced hormonal machine that is highly sensitive to change and just because you were ok to colour your once done not always mean that it will be the same next time.
Colour Care Active Botanicals


DENOXYLINE
(Green Tea) A purified fraction of green tea polyphenols, Denoxyline is a powerful quencher of free radicals. Thanks to its anti-oxidant and chelating activities, it is able to protect the hair colour efficiently against external stress.


SWEET ALMOND OIL
Rich in Oleic and linoleic fatty acids and containing Vitamins A, B1, B2 and B6; this oil is used for its penetrating, smoothing, softening and moisturising properties for dry and brittle hair.


HYDROMIST L
(Blue Lupine): A plant based peptide solution made by enzymatic hydrolysis of lupine proteins and used as a gluten free film former to improve hair condition.










