Hair Science, Hair Loss Men, Hair Loss Women
SCALP COOLING IN CHEMOTHERAPY
Chemotherapy-induced alopecia continues to be a psychologically distressing side-effect for the cancer patient undergoing treatment. Depending on the degree of importance placed on hair by the patient, alopecia can cause negative changes in body image, decrease social activity, alter interpersonal relationships and add enormous additional stress. Scalp cooling has long been a controversial issue due to conflicting reports on its efficacy, but many of the published criticisms are largely due to an inadequate understanding of the procedure. There is no longer any doubt that scalp cooling is effective for many patients, but the selection of patients may be a crucial issue.
INTRODUCTION: THE RATIONALE
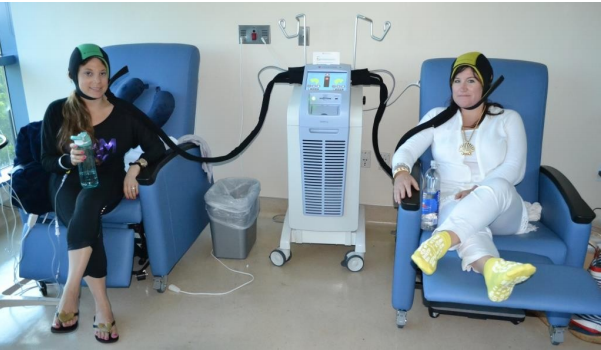
 Alopecia, or loss of scalp hair, is a common side effect of many drugs. It may be partial or complete and may last a variable length of time. Although many different chemical agents can cause or contribute to hair loss, it is the chemotherapeutic agents used for treating cancer that regularly cause alopecia. Many attempts have been made to reduce the alopecia produced upon the administration of chemotherapeutic agents. Many of these efforts have been aimed at reducing the blood flow and thus probable delivery of the drug to the scalp. Various devices such as cryopacks and cooling caps have been utilised. This cooling is applied prior to, during, and for a time following infusion of the drug and is able to decrease scalp blood flow to 35 per cent of the baseline. Numerous research studies have attempted to confirm the efficacy of scalp cooling, but the evidence until recently has been inconclusive. However, despite these inconsistencies it is clear that many patients experience reduced alopecia after scalp cooling. Minimising alopecia contributes to improvements in patients’ self-esteem and perception of body image, which are considered important in the management of their disease. There are many reasons for scalp-cooling failing to deliver protection from alopecia, including inappropriate selection of patients, variable patient responses to treatment, the different methods of scalp cooling, variation in liver function between patients, and different drug regimes. While, in theory, impaired liver function could reduce the metabolism and excretion of the drug, leading to an increased risk of alopecia, certain studies have obtained very good hair preservation despite high incidence of liver metastases. Further studies are perhaps indicated.
Alopecia, or loss of scalp hair, is a common side effect of many drugs. It may be partial or complete and may last a variable length of time. Although many different chemical agents can cause or contribute to hair loss, it is the chemotherapeutic agents used for treating cancer that regularly cause alopecia. Many attempts have been made to reduce the alopecia produced upon the administration of chemotherapeutic agents. Many of these efforts have been aimed at reducing the blood flow and thus probable delivery of the drug to the scalp. Various devices such as cryopacks and cooling caps have been utilised. This cooling is applied prior to, during, and for a time following infusion of the drug and is able to decrease scalp blood flow to 35 per cent of the baseline. Numerous research studies have attempted to confirm the efficacy of scalp cooling, but the evidence until recently has been inconclusive. However, despite these inconsistencies it is clear that many patients experience reduced alopecia after scalp cooling. Minimising alopecia contributes to improvements in patients’ self-esteem and perception of body image, which are considered important in the management of their disease. There are many reasons for scalp-cooling failing to deliver protection from alopecia, including inappropriate selection of patients, variable patient responses to treatment, the different methods of scalp cooling, variation in liver function between patients, and different drug regimes. While, in theory, impaired liver function could reduce the metabolism and excretion of the drug, leading to an increased risk of alopecia, certain studies have obtained very good hair preservation despite high incidence of liver metastases. Further studies are perhaps indicated.
Trichological Considerations

Cancer chemotherapy exerts its effect not only upon malignant cells but also upon normal cells, which have a high mitotic activity, for example the hair bulbs of anagen follicles. At any given time, 90 per cent of human hair follicles are in the anagen or actively dividing phase. It is this large proportion of hair follicles that is susceptible to chemotherapy’s deleterious effects. Hair loss from chemotherapy occurs either by total atrophy and loss of the hair bulb or, more frequently, by partial atrophy of the bulb causing constriction of the hair shaft.1 The hair shaft then breaks off easily with any trauma such as washing or combing.
Alopecia induced by chemotherapy is reversible. Regeneration of hair growth occurs within one to two months after discontinuation of therapy.
Cooling Times
The degree of protection against hair loss is inversely proportional to the dose of alopecia inducing drug being administered2 , therefore high dose single agent or combination regimes would have a longer post infusion cooling time than low dose regimes. Tolerance and Side Effects The most common complaints are discomfort, light-headedness after the cooling cap has been removed and a smaller number of patients experience headaches.
1 Crouse, R.G Van Scott, E.J: Changes in scalp hair roots as a measure of toxicity from cancer chemotherapy drugs.
J Invest Dermatol 35: 83-90, 1960
2 Tollenaar et al: Scalp cooling has no place in the prevention of alopecia in adjuvant chemotherapy for breast cancer. Eur J. Cancer 1994, 30A, 1448-1453 Patients may experience feeling cold during the first 10 minutes of pre-cooling but studies have shown that most patients become accustomed to the low temperatures for the rest of the treatment period.
Volume-ise / Hairfood Active Botanicals


GINGKO
Working with Kigalia and Clary as an original blend of 3 plants acting synergistically and allowing scalp toning and limiting hair loss. They act on factors avoiding hair loss including 5-alpha-reductase inhibition, scalp microcirculation improvement and to decrease inflammation contributing to Seborrhoea (oiliness) which can block scalp follicles inhibiting growth.


KIGALIA AFRICANA
Working with Gingko and Clary as an original blend of 3 plants acting synergistically and allowing scalp toning and limiting hair loss . They act on factors avoiding hair loss including 5-alpha-reductase inhibition, scalp microcirculation improvement and to decrease inflammation contributing to Seborrhoea (oiliness) which can block scalp follicles inhibiting growth.


CLARY
Working with Kigalia and Gingko as an original blend of 3 plants acting synergistically and allowing scalp toning and limiting hair-loss. They act on factors avoiding hair loss including 5-alpha-reductase inhibition, scalp microcirculation improvement and to decrease inflammation contributing to Seborrhoea (oiliness) which can block scalp follicles inhibiting growth.